There is a large shortfall in women’s health services in the UK; with awareness, education and access to treatment falling far behind Scandinavia and other European countries.
The incidence of women’s health issues in the UK is huge. 1 in 3 women have urinary incontinence, 1 in 12 have faecal incontinence and 8 out of 10 women experience invasive menopause symptoms, to list just 3 examples. The scale of the issues is only matched by the lack of support available. (For context, of the 16 million women going through menopause or perimenopause fewer than 1.5% are on HRT, even though it’s safe for most women.)
At Ten, we think women have put up with this for too long. We believe that women deserve evidence-based advice and treatment. Women should not have to suffer in silence or feel embarrassed. And we – Ten’s specialists in Women’s Health Physiotherapy – are here to help.
Here are 10 of the most common pelvic health issues that most women don’t know that they can get better help with.
1. Feeling unsure or lost about how to do pelvic floor exercises, whilst being told they’re incredibly important and must be done correctly
Your pelvic floor controls your bladder, bowel, sexual function, supports your internal organs, stabilises your pelvis and rotates your baby’s head during labour. Recent UK Guidelines suggest that pelvic floor exercises should be taught to girls in school to prevent pelvic floor issues developing in the future. Recent studies indicate that up to 70% of women do not complete pelvic floor exercises correctly – and this widespread lack of understanding of how to perform pelvic floor exercise is inextricably linked to the lack of awareness of who to go to for help. Most women don’t even know that there is such a thing as pelvic floor physiotherapy, let alone that a suitable qualified Physio can show you the correct technique, and can tailor your exercise programme to suit your individual needs, as every pelvic floor is different.
2. Constipation
Persistent constipation isn’t always linked to diet (though we’re usually told that it is). Tension in the pelvic floor encourages the body to store faeces for longer than needed, resulting in constipation and straining when emptying your bowel. Haemorrhoids and anal fissures are a tell-tale sign that you have pelvic floor tension. Pelvic health physiotherapy treatment can reduce the muscle tension and help to regulate your bowels long-term.
3. Painful Periods
Painful periods are too often dismissed as being a normal part of life. They are common, but they’re not normal. There are lots of different reasons why women get painful periods. Our lifestyle choices, stress and inflammatory levels, pelvic muscle strength and length, pelvic floor health, choice of exercise during our cycle and daily habits can all contribute. Hormonal contraception can help some women, but not all. Pelvic health physiotherapy looks holistically at your symptoms, identifies the triggers and shows you effective ways to treat your pain.
4. Being told that you’re not perimenopausal because you’re still having periods
Many women are frustrated at being told they are not perimenopausal when they clearly have bothersome, and sometimes life-changing symptoms. Admittedly, perimenopause is difficult to diagnose and is not dependent on hormone testing or your periods – you can still have regular periods and normal blood hormone levels, and still be perimenopausal. But that doesn’t mean you have to accept what you’re told, especially when you suspect it’s wrong. An accurate diagnosis of perimenopause – and an effective treatment plan – can be made by reviewing your symptoms and trialling different treatments to regulate your hormones.
5. Being told that it’s ok to run at 6 weeks postnatal (it most certainly is not)
Your ligaments and connective tissue in your abdomen take time to heal and recover. This takes a minimum of 12 weeks. It is safe to start body weight exercises and light weights if it feels comfortable, but you should not run or do any high intensity training within the first 12 weeks of giving birth.
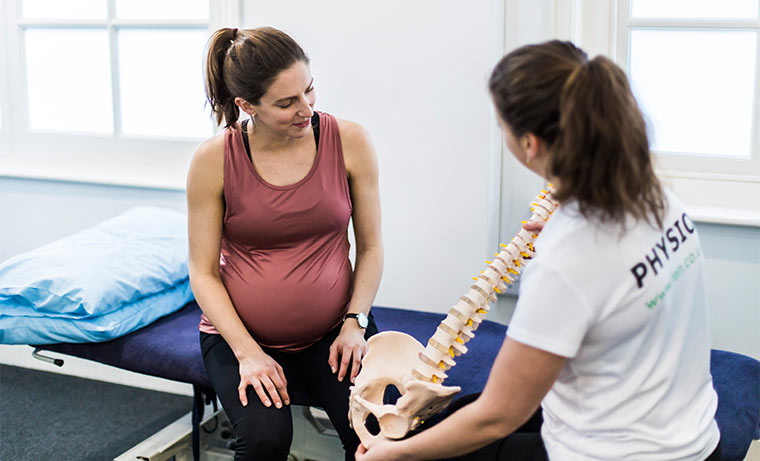
6. Being told that pelvic pain during pregnancy is normal and just related to your hormones
Pelvic pain is common during pregnancy and caused by a number of different factors, such as pelvic position, sleep, stress levels, joint mobility, daily postures, activity levels (too much or too little), strength and muscular endurance. Pelvic health physiotherapy can address these issues and treat your symptoms to ensure you can stay fit and active throughout your pregnancy.
7. Worrying you’ll leak when you cough, sneeze or laugh
1 in 3 women have incontinence. The issue often starts after having a baby or going through the menopause, although it can start as early as your teenage years. Many have come to expect symptoms of incontinence and have been told that there is nothing that can be done. This is wrong, and a failure on the part of the health system. Pelvic health physiotherapy alone can resolve up to 75% of bothersome symptoms. If the issue can’t be resolved with physiotherapy alone, our pelvic health Physiotherapists will explain the other non-invasive options available.
8. Being sent home after having a baby without understanding how to care for your stitches or what to expect from the next 6 weeks
Many women report that the information they receive after having a baby doesn’t adequately prepare or inform them about what to expect in the postnatal period. Women are unsure what is normal and what’s not, and there is very little focus on the well-being of the mother as she recovers. Persistent perineal and vaginal pain, vaginal heaviness, incontinence, abdominal separation and pain are a few of the symptoms that women report. Postnatal GP checks are brief and often focused on the health of the baby. Our Postnatal MOTs screen you for postnatal complications, including vaginal and pelvic floor health, abdominal separation (rectus abdominis diastasis) and address any pain that you may be experiencing. Our experts will get you back to feeling yourself again.
9. Not being told that your perineal length (length of the area between your vagina and rectum) is directly related to your risk of serious tears during vaginal delivery
Perineal body length is a good predictor of your risk of sustaining a serious grade 3 or 4 perineal tear. Grade 3 and 4 tears run from the vagina to the rectum and can lead to both bladder and bowel incontinence. 3 in 100 women will sustain a tear of this nature during vaginal delivery. All women should have their perineums measured if they’re planning a vaginal delivery to assess their risk of sustaining a serious tear. This information can then be used by your midwife and obstetrician to develop your birthing plan. Unfortunately, perineal measuring is not routinely carried out in the NHS during pregnancy. Our prenatal MOTs measure your perineal length, teach you perineal massage techniques that can reduce the risk of tearing by 20%, and fully prepare you for labour and the postnatal period.
10. Suffering with incontinence after having chemotherapy or radiotherapy and not being told that this can be treated
Radiotherapy and chemotherapy can weaken the pelvic floor and lead to bladder and bowel incontinence, as well as vaginal sensitivity and pain. Pelvic floor physiotherapy strengthens your pelvic floor muscles and addresses the sensitivity. We can also advise you on how to get back into physical activity and strengthen the muscles that work with the pelvic floor for optimum recovery.

